Check out today’s Step 2 CK Qmax Question Challenge.
Know the answer? Post it in the comments below! Don’t forget to check back for an update with the correct answer and explanation (we’ll post it in the comments section below).
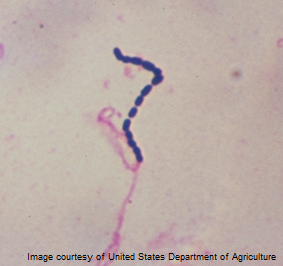 A 32-year-old woman is brought to the emergency department by her husband because of increased lethargy along with a headache, high fever, and new purpuric lesions. One year ago she underwent splenectomy for idiopathic thrombocytopenic purpura (ITP) that failed prednisone therapy. The patient is allergic to ?-lactam agents. Her temperature is 39.6°C (103.2°F), blood pressure is 102/64 mm Hg, pulse is 124/min, and respiratory rate is 19/min. The patient’s husband recalls she had a minor upper respiratory tract infection the previous week that seemed to resolve on its own. On examination the patient is ill appearing, in respiratory distress, and confused. Blood culture reveals gram-positive cocci in chains (see image).
A 32-year-old woman is brought to the emergency department by her husband because of increased lethargy along with a headache, high fever, and new purpuric lesions. One year ago she underwent splenectomy for idiopathic thrombocytopenic purpura (ITP) that failed prednisone therapy. The patient is allergic to ?-lactam agents. Her temperature is 39.6°C (103.2°F), blood pressure is 102/64 mm Hg, pulse is 124/min, and respiratory rate is 19/min. The patient’s husband recalls she had a minor upper respiratory tract infection the previous week that seemed to resolve on its own. On examination the patient is ill appearing, in respiratory distress, and confused. Blood culture reveals gram-positive cocci in chains (see image).
Which of the following therapies is most appropriate to treat this patient’s underlying infection?
A. Cefepime
B. Gentamicin
C. Levofloxacin
D. Nafcillin
E. Penicillin
______________________
Want to know the ‘bottom line?’ Purchase a USMLE-Rx Subscription and get many more features, more questions, and passages from First Aid for the USMLE Step 2 CK, including images, references, and other facts relevant to this question.
This practice question is an actual question from the USMLE-Rx Step 2 CK test bank. Get more Step 2 CK study help at USMLE-Rx.com.



C) Levoflox
A Respiratory Fluoroquinolone
C
Levofl
agree
C. Gram-positive streptococcus.
The correct answer is C. This patient has postsplenectomy sepsis. Splenectomy is indicated in patients with idiopathic thrombocytopenic purpura (ITP) who fail traditional medical therapy with glucocorticoids after 4–6 weeks. Following splenectomy, about 66% of patients with ITP recover to a normal platelet count. The spleen is the major site of destruction of antibody-sensitized platelets. In addition, the spleen is involved in the clearance of bacteria, specifically encapsulated bacteria such as Streptococcus pneumoniae, Haemophilus influenzae type b, and Neisseria meningitidis. Recommended empiric therapy for postsplenectomy sepsis is broad-spectrum antibiotics: combination of IV vancomycin and ceftriaxone.
S. pneumonia infection accounts for the majority of cases of postsplenectomy sepsis and is the most likely cause in this case. Treatment for S. pneumoniae is third-generation cephalosporins like ceftriaxone or cefotaxime, but this patient is allergic to ?-lactam agents. In patients with allergy to penicillin and cephalosporins, aztreonam, ciprofloxacin, or levofloxacin can be used.
A is not correct. Cefepime is useful in treating bacteremia due to Pseudomonas aeruginosa. However, P. aeruginosa is not an encapsulated bacteria and has not been associated with postsplenectomy sepsis. Streptococcus pneumoniae accounts for the majority of postsplenectomy sepsis cases. Cefepime is not indicated for postsplenectomy sepsis.
B is not correct. Gentamicin may be used to treat infections with gram-negative organisms and bacteremia due to viridans streptococci. However, viridans streptococci are not encapsulated organisms and would not be expected to be the most likely cause of this patient’s symptoms. Although Streptococcus pneumoniae and viridans streptococci are both ?-hemolytic gram-positive cocci that are found in chains, it is S. pneumoniae that accounts for the majority of postsplenectomy sepsis cases.
D is not correct. Nafcillin would be an appropriate therapy for Staphylococcus aureus in a patient without a ?-lactam allergy. Alternatively, a fluoroquinolone could be used to treat a suspected S. aureus infection. However, S. aureus is not usually involved in postsplenectomy sepsis because it is not an encapsulated bacterium. In addition, this gram-positive organism is often found in clusters rather than in chains.
E is not correct. In the absence of a ?-lactam allergy, penicillin would be an appropriate therapy in suspected Neisseria meningitidis infection. Although N. meningitidis is an encapsulated bacterium that may cause sepsis in patients who have had a splenectomy, Streptococcus pneumoniae accounts for the majority of cases of postsplenectomy sepsis and is therefore much more likely to be involved in this case than is N. meningitidis. In addition, N. meningitidis is a gram-negative diplococcus and is therefore not supported by the microbiology obtained.