Check out today’s Step 1 Qmax Question Challenge.
Know the answer? Post it below! Don’t forget to check back for an update with the correct answer and explanation (we’ll post it in the comments section below).
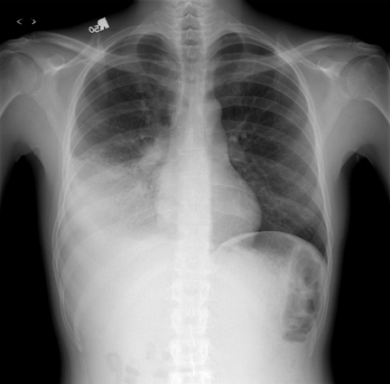 An 82-year-old woman with chronic obstructive pulmonary disease (COPD) is hospitalized for an acute COPD exacerbation. On admission the patient is found to have a pH of 7.25 and PaCO2 of 50. She is rapidly placed on ventilatory support and admitted to the ICU. After being on the ventilator for 72 hours, the patient is found to have a temperature of 102°F (38.9°C), pulse of 104/min, and BP of 115/20 mm Hg. Labs are significant for a white blood cell count of 15,000 cells/?L. A chest X-ray is taken and is shown. Sputum studies are significant for a gram-negative bacillus Acinetobacter baumannii. She is treated with intravenous antibiotics, but several hours later the patient has a seizure lasting 45 seconds. A subsequent lumbar puncture is normal. The physician suspects a pharmacologic cause for the seizure.
An 82-year-old woman with chronic obstructive pulmonary disease (COPD) is hospitalized for an acute COPD exacerbation. On admission the patient is found to have a pH of 7.25 and PaCO2 of 50. She is rapidly placed on ventilatory support and admitted to the ICU. After being on the ventilator for 72 hours, the patient is found to have a temperature of 102°F (38.9°C), pulse of 104/min, and BP of 115/20 mm Hg. Labs are significant for a white blood cell count of 15,000 cells/?L. A chest X-ray is taken and is shown. Sputum studies are significant for a gram-negative bacillus Acinetobacter baumannii. She is treated with intravenous antibiotics, but several hours later the patient has a seizure lasting 45 seconds. A subsequent lumbar puncture is normal. The physician suspects a pharmacologic cause for the seizure.
The patient’s adverse reaction was most likely caused by which of the following antibiotics?
A. Gentamicin
B. Imipenem
C. Levofloxacin
D. Linezolid
E. Rifampin
———————–
Want to know the ‘bottom line?’ Purchase a USMLE-Rx Subscription and get many more features, more questions, and passages from First Aid, including images, references, and other facts relevant to this question.
This practice question is an actual question from the USMLE-Rx Step 1 test bank. For more USMLE Step 1 prep, subscribe to our Flash Facts and Step 1 Express video series. Score the best deal on all three products with USMLE-Rx 360 Step 1.




ans :B
B
B
imipenem
Choice B, it is!
B. Imipinem is a drug of choice for A. baumanii infection. 2nd line antibiotics are: sulbactam, tigecycline, polymyxin B
The correct answer is B. The patient has a COPD exacerbation as demonstrated by the significant respiratory acidosis on arterial blood gas measurements. The patient is put on a ventilator and 72 hours later found to be febrile and tachycardic with an elevated WBC count and a new right lower lobe consolidation. These signs are all concerning for a ventilator-associated pneumonia. The patient is found to have Acinetobacter baumannii on sputum culture and is started on antibiotics. Several hours after starting the IV antibiotic, the patient has a seizure, with normal lumbar puncture, indicating a likely drug side effect.
Antibiotic-related seizure complications, although not common, are most often associated with ?-lactams. Imipenem is a broad-spectrum, ?-lactamase-resistant antibiotic of the carbapenem class and is structurally similar to ?-lactam antibiotics. It is administered with cilastatin, which helps to decrease renal metabolism of imipenem, and thus increase its half-life. Carbapenems can be used to treat both gram-positive and gram-negative infections, and it is first-line therapy in the treatment of Acinetobacter and Enterobacter species infections. Imipenem is not useful in treating infections caused by methicillin-resistant Staphylococcus aureus, Enterococcus faecium, or Staphylococcus epidermidis. Adverse effects include gastrointestinal distress, thrombophlebitis, skin rashes, and seizures.
Gentamicin and rifampin do not cause seizures. Levofloxacin and Linezolid may lower seizure threshold, but are not typically used to treat Acinetobacter infections.
A is not correct. Gentamicin is an aminoglycoside antibiotic used to treat gram-negative bacilli and works by inhibiting protein synthesis. Adverse effects include nephrotoxicity, ototoxicity, and neuromuscular blockade. Gentamicin is effective in treating Acinetobacter species infection, but it is not the first-line choice. It is not associated with seizures.
C is not correct. Levofloxacin is a fluoroquinolone antibiotic that acts by inhibiting DNA gyrase. It is used to treat infections from gram-negative rods and some gram-positive organisms and therefore is good for upper respiratory infections and urinary tract infections. Fluoroquinolones are generally well tolerated but are associated with anaphylaxis, gastrointestinal discomfort, headache, and phototoxicity. They are also associated with damaged cartilage in animal models and thus are contraindicated in children. Other fluoroquinolones, such as ciprofloxacin, may lower the seizure threshold in some patients, but are not typically used in treating Acinetobacter infections.
D is not correct. Linezolid is used for community-acquired pneumonias and acts by binding to the bacterial 50S ribosomal RNA subunit and blocking protein synthesis. Adverse effects include gastrointestinal upset, headache, and myelosuppression. Linezolid is a weak monoamine oxidase inhibitor (MAOI) and should be used with caution in the setting of MAOIs and serotonin reuptake inhibitors because there is concern for serotonin syndrome. Although there is evidence that linezolid can lower the seizure threshold, it is not used for managing infections with gram-negative pathogens and, consequently, is not the single best answer.
E is not correct. Rifampin is used as prophylaxis in individuals exposed to Neisseria meningitidis and to treat tuberculosis. It acts by inhibiting DNA-dependent RNA polymerase. Important adverse effects include a transient rise in hepatic aminotransferase levels (which usually return to normal without discontinuation of rifampin) and hepatitis, which can occur directly or due to rifampin exacerbating the hepatotoxicity of other drugs. Rifampin also causes discoloration of body fluids, so patients should be cautioned that their tears and urine may turn orange-red. It does not cause seizures.